Clubfoot
| Clubfoot | |
|---|---|
| Synonyms | Clubfoot, congenital talipes equinovarus (CTEV)[1] |
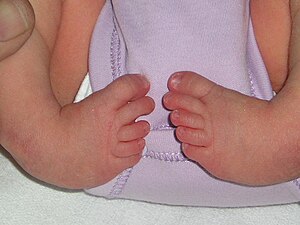 | |
| Bilateral clubfoot | |
| Specialty | Orthopedics |
| Symptoms | Foot that is rotated inwards[1] |
| Usual onset | During early pregnancy[1] |
| Causes | Unknown[1] |
| Risk factors | Genetics, mother who smokes cigarettes[1] |
| Diagnostic method | Examination, ultrasound[1][2] |
| Differential diagnosis | Metatarsus adductus[3] |
| Treatment | Ponseti method (manipulation, casting, cutting the Achilles tendon, braces), French method, surgery[1][2] |
| Prognosis | Good with treatment[2] |
| Frequency | 1 in 1,000[2] |
Clubfoot is a birth defect where one or both feet are rotated inwards and downwards.[1][4] The affected foot, calf and leg may be smaller than the other.[1] In about half of those affected, both feet are involved.[1] Most cases are not associated with other problems.[1] Without treatment, people walk on the sides of their feet, which causes problems with walking.[2]
The exact cause is usually unclear.[1] A few cases are associated with distal arthrogryposis or myelomeningocele.[2] If one identical twin is affected, there is a 33% chance the other one will be as well.[1] Diagnosis may occur at birth or before birth during an ultrasound exam.[1][2]
Initial treatment is most often with the Ponseti method.[1] This involves moving the foot into an improved position followed by casting, which is repeated at weekly intervals.[1] Once the inward bending is improved, the Achilles tendon is often cut, and braces are worn until the age of four.[1] Initially, the brace is worn nearly continuously and then just at night.[1] In about 20% of cases, further surgery is required.[1]
Clubfoot occurs in about 1 in 1,000 newborns.[2] The condition is less common among the Chinese and more common among the Māori.[2] Males are affected about twice as often as females.[1] Treatment can be carried out by a range of healthcare providers and can generally be achieved in the developing world with few resources.[1]
Contents
1 Signs and symptoms
2 Cause
2.1 Genetics
3 Diagnosis
4 Treatment
4.1 Ponseti method
4.2 French method
4.3 Surgery
5 History
6 Society and culture
6.1 Literature and film
7 References
8 External links
Signs and symptoms
In clubfoot, one or both feet are rotated inwards and downwards.[1][4] The affected foot, calf, and leg may be smaller than the other.[1] In about half of those affected, both feet are involved.[1] Most cases are not associated with other problems.[1] Without treatment, people walk on the sides of their feet, which causes issues with walking.[2]
Cause
There are many hypotheses about how clubfoot develops. Some hypothesis include: environmental factors, genetics, or a combination of both. Research has not yet pinpointed the root cause, but many findings agree that "it is likely there is more than one different cause and at least in some cases the phenotype may occur as a result of a threshold effect of different factors acting together."[5]
Some researchers hypothesize, from the early development stages of humans, that clubfoot is formed by a malfunction during gestation. Early amniocentesis (11–13 wks) is believed to increase the rate of clubfoot because there is an increase in potential amniotic leakage from the procedure.[citation needed] Underdevelopment of the bones and muscles of the embryonic foot may be another underlying cause. In the early 1900s, it was thought that constriction of the foot by the uterus contributed to the occurrence of clubfoot.[citation needed]
Underdevelopment of the bones also affects the muscles and tissues of the foot. Abnormality in the connective tissue causes "the presence of increased fibrous tissue in muscles, fascia, ligaments and tendon sheaths".[5]
Genetics
Mutations in genes involved in muscle development are risk factors for clubfoot, specifically those encoding the muscle contractile complex (MYH3, TPM2, TNNT3, TNNI2 and MYH8). These can cause congenital contractures, including clubfoot, in distal arthrogryposis (DA) syndromes.[6] Clubfoot can also be present in people with genetic conditions such as Loeys–Dietz syndrome.
Genetic mapping and the development of models of the disease have improved understanding of developmental processes. Its inheritance pattern is explained as a heterogenous disorder using a polygenic threshold model. The PITX1-TBX4 transcriptional pathway has become key to the study. PITX1 and TBX4 are uniquely expressed in the hind limb.[7]
Diagnosis
Diagnosis of clubfoot deformity is by physical examination. Typically, a newborn is examined shortly after delivery with a head to toe assessment. Examination of the lower extremity and foot reveals the deformity, which may affect one or both feet. Examination of the foot shows four components of deformity.
- First, there is a higher arch on the inside of the foot. This component of the deformity can occur without the other aspects of clubfoot deformity. In isolation, this aspect of the deformity is called cavus deformity.
- Second, the forefoot is curved inward or medially (toward the big toe). This component of the deformity can occur without the other aspects of clubfoot deformity. In isolation, this aspect of the deformity is called metatarsus adductus.
- Third, the heel is turned inward. This is a natural motion of the heel and subtalar joint, typically referred to as inversion. In clubfoot deformity, the turning in (inversion) of the heel is fixed (not passively correctable) and considered a varus deformity.
- Fourth, and finally, the ankle is pointed downward. This is a natural motion of the ankle referred to as plantar flexion. In clubfoot deformity, this position is fixed (not correctable) and is referred to as equinus deformity.
A foot that shows all four components is diagnosed as having clubfoot deformity. These four components of a clubfoot deformity can be remembered with the acronym CAVE (cavus, forefoot adductus, varus and equinus).
The severity of the deformity can also be assessed on physical exam, but is subjective to quantify. One way to assess severity is based on the stiffness of the deformity or how much it can be corrected with manual manipulation of the foot to bring it into a corrected position. Other factors used to assess severity include the presence of skin creases in the arch and at the heel and poor muscle consistency.
In some cases, it may be possible to detect the disease prior to birth during a prenatal ultrasound. Prenatal diagnosis by ultrasound can allow parents the opportunity to get information about this condition and make plans for treatment after their baby is born.[8]
Other testing and imaging is typically not needed. Further testing may be needed if there are concerns for other associated conditions.
Treatment

Clubfeet in the course of correcting
Treatment is usually with some combination of the Ponseti or French methods.[2] The Ponseti method includes the following: casting together with manipulation, cutting the Achilles tendon, and bracing. The Ponseti method has been found to be effective in correcting the problem in those under the age of two.[9] The French method which involves realignment and taping of the foot is often effective but requires a lot of effort by caregivers.[2] Another technique known as Kite does not appear as good.[10] In about 20% of cases, further surgery is required.[1]
Ponseti method

A foot abduction brace type Denis Browne bar. Various types of foot-abduction braces are used to hold the child's feet in the desired position.
Using the Ponseti method, the foot deformity is corrected in stages. These stages are as follows: manipulating the foot to an improved position and then holding it with a long leg cast, then removing the cast after a week, and then manipulating the foot again. The foot position usually improves over a course of 4–6 casts. The amount of casts varies from person to person to address each individual's characteristic needs.
- The initial cast focuses on aligning the forefoot with the hindfoot as Ponseti describes the forefoot as relatively pronated in comparison to the hindfoot. Supinating the forefoot and elevating the first metatarsal improves this alignment.
- Subsequent casts are applied after stretching the foot with a focus on abducting the forefoot with lateral pressure at the talus, to bring the navicula laterally and improve the alignment of the talonavicular joint. In contrast to the Kite Method of casting, it is important to avoid constraining the calcanocuboid joint. With each additional cast, the abduction is increased and this moves the hindfoot from varus into valgus. It is important to leave the ankle in equinus until the forefoot and hindfoot are corrected.
- The final stage of casting, is to correct the equinus. After fully abducting the forefoot with spontaneous correction of the hindfoot, an attempt is made to bring the ankle up and into dorsiflexion. For the majority of children, the equinus will not fully correct with casting and a procedure is done to facilitate this final aspect of the deformity correction. The procedure is a percutaneous heel cord release or tenotomy. Ponseti advocated for doing this in the clinic with a local anesthetic. For safety reasons, many centers perform this procedure with sedation or monitored anesthesia care. In this procedure, numbing medicine is applied, the skin is cleansed, and a small scalpel is used to divide the Achilles tendon. With a small scalpel there is minimal bleeding and no need for stitches. A small dressing is applied and a final clubfoot cast is applied with the foot in a fully corrected position. This cast is typically left in place for 3 weeks.
After correction has been achieved with casting, maintenance of correction starts with full-time (23 hours per day) use of a brace —also known as a foot abduction brace (FAB)—on both feet, regardless of whether the TEV is on one side or both, typically full-time for 3 months. After 3 months, brace wear is decreased and used mostly when sleeping for naps and at night-time. This part-time bracing is recommended until the child is 4 years of age.
Roughly 30% of children will have recurrence. A recurrence can usually be managed with repeating the casting process. Recurrence is more common when there is poor compliance with the bracing, because the muscles around the foot can pull it back into the abnormal position. Approximately 20% of infants successfully treated with the Ponseti casting method will have an imbalance between the muscles that invert the ankle (posterior tibialis and anterior tibialis muscles) and the muscles that evert the ankle (peroneal muscles). Patients with this imbalance are more prone to recurrence. After 18 months of age, this can be addressed with surgery to transfer the anterior tibialis tendon from it medial attachment (the navicula) to a more lateral position (the lateral cuneiform) to rebalance these muscle forces. While this requires a general anesthetic and subsequent casting while the tendon heals, it is a relatively minor surgery that corrects a persistent muscle imbalance while avoiding disturbance to the joints of the foot.
French method
The French method for treatment of clubfoot is a conservative method of treatment of a newborn which requires daily physical therapy for the first two months. The goal of this treatment is to avoid future need of surgery, but the success rate varies and after release surgery may still be necessary. The treatment includes daily manipulations of the feet along with stretching of the feet, followed by taping in order to maintain the range of motion gains achieved at the end of each session. The French method differs from the Ponseti method in that the taping techniques allow some motion in the feet. Another focus is to strengthen the peroneal muscles which is thought to contribute towards long-term correction. After the two month mark physical therapy sessions can be weaned down to three times per week instead of daily until the child reaches six months old. Parents are required to continue on with home exercises and night splinting even after the program has achieved proper foot correction in order to maintain the correction. The Ponseti method is generally preferred.[2]
Surgery
If non-operative treatments are unsuccessful or achieve incomplete correction of the deformity, surgery is sometimes needed. Surgery was more common prior to the widespread acceptance of the Ponseti Method. The extent of surgery depends on the severity of the deformity. Usually, surgery is done at 9 to 12 months of age and the goal is to correct all the components of the clubfoot deformity at the time of surgery.
For feet with the typical components of deformity (cavus, forefoot adductus, hindfoot varus, and ankle equinus), the typical procedure is a Posteromedial Release (PMR) surgery. This is done through an incision across the medial side of the foot and ankle, that extends posteriorly, and sometimes around to the lateral side of the foot. In this procedure, it is typically necessary to release (cut) or lengthen the plantar fascia, several tendons, and joint capsules/ligaments. Typically, the important structures are exposed and then sequentially released until the foot can be brought to an appropriate plantigrade position. Specifically, it is important to bring the ankle to neutral, the heel into neutral, the midfoot aligned with the hindfoot (navicula aligned with the talus, and the cuboid aligned with the calcaneus). Once these joints can be aligned, thin wires are usually placed across these joints to hold them in the corrected position. These wires are temporary and left out through the skin for removal after 3–4 weeks. Once the joints are aligned, tendons (typically the Achilles, posterior tibialis, and flexor halluces longus) are repaired at an appropriate length. The incision (or incisions) are closed with dissolvable sutures. The foot is then casted in the corrected position for 6–8 weeks. It is common to do a cast change with anesthesia after 3–4 weeks, so that pins can be removed and a mold can be made to fabricate a custom AFO brace. The new cast is left in place until the AFO is available. When the cast is removed, the AFO is worn to prevent the foot from returning to the old position.[8]
For feet with partial correction of deformity with non-operative treatment, surgery may be less extensive and may involve only the posterior part of the foot and ankle. This might be called a posterior release. This is done through a smaller incision and may involve releasing only the posterior capsule of the ankle and subtalar joints, along with lengthening the Achilles tendon.
Surgery leaves residual scar tissue and typically there is more stiffness and weakness than with nonsurgical treatment. As the foot grows, there is potential for asymmetric growth that can result in recurrence of foot deformity that can affect the forefoot, midfoot, or hindfoot. Many patients do fine, but some require orthotics or additional surgeries. Long-term studies of adults with post-surgical clubfeet, especially those needing multiple surgeries, show that they may not fare as well in the long term, according to Dobbs, et al.[11] Some patients may require additional surgeries as they age, though there is some dispute as to the effectiveness of such surgeries, in light of the prevalence of scar tissue present from earlier surgeries.
History
Treatment of clubfoot is evident as early as Egyptian paintings. In early days,[when?] the foot was manipulated with a Thomas wrench and casting which caused fracture of several bones in the foot. Hippocrates around 400 B.C. was the first to offer a medical explanation.
Society and culture

Famous storyteller from Lapland. Juho "Nätti-Jussi" Nätti (surname can be translated as "pretty") who lived 1890-1964, was known for his stories but also his untreated left clubfoot. A story tells that "not even the devil himself could tell which way Nätti has gone" from the footprints of snow.
Literature and film
- The main character, Philip Carey, in W. Somerset Maugham's novel Of Human Bondage, has clubfoot, a central theme in the work.
- Hippolyte Tautain, the stableman at the Lion D'Or public house in Gustave Flaubert's novel Madame Bovary is unsuccessfully treated for clubfoot by Charles Bovary, leading to the eventual amputation of his leg.
- Charlie Wilcox, the main character in Sharon McKay's novel Charlie Wilcox had a clubfoot.
- In Yukio Mishima's seminal novel The Temple of the Golden Pavilion the character Kashiwagi has clubfoot which parallels the stutter of the main character, Mizoguchi.
- In David Eddings' Malloreon series, Senji the sorcerer has a clubfoot.
- In Caroline Lawrence's Roman Mysteries series, a character called Vulcan the blacksmith appears in the book "The Secrets of Vesuvius". He reveals that he gained the nickname because of his clubfoot.
- In Bernard Cornwell's The Warlord Chronicles Mordred, King of Dumnonia, has clubfoot that is often used as a symbol for his ugliness and weakness as a ruler.
- In Daniel Keyes's Flowers for Algernon Gimpy, one of Charlie's co-workers at the bakery, has clubfoot.
- In Perfume: The Story of a Murderer, the main character is born with clubfoot and is described as having a limp throughout the novel.
- In Flannery O'Connor's short story "The Lame Shall Enter First", the character Johnson has clubfoot, a major symbol of the story.
- Kwai Geuk-Chat, played by Hung Yan-yan, was the former antagonist and later new student of Wong Fei-hung in the Once Upon a Time in China franchise was nicknamed "Clubfoot Seven Chiu-Tsat" due to the shape of the disability and deformation of his feet as he is the 7th member of wealthy rival martial artist, Chiu Tin-bak's apprentices, disciples and henchmen.
References
^ abcdefghijklmnopqrstuvwxyz Gibbons, PJ; Gray, K (September 2013). "Update on clubfoot". Journal of paediatrics and child health. 49 (9): E434–7. doi:10.1111/jpc.12167. PMID 23586398..mw-parser-output cite.citation{font-style:inherit}.mw-parser-output q{quotes:"""""""'""'"}.mw-parser-output code.cs1-code{color:inherit;background:inherit;border:inherit;padding:inherit}.mw-parser-output .cs1-lock-free a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/6/65/Lock-green.svg/9px-Lock-green.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .cs1-lock-limited a,.mw-parser-output .cs1-lock-registration a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/d/d6/Lock-gray-alt-2.svg/9px-Lock-gray-alt-2.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .cs1-lock-subscription a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/a/aa/Lock-red-alt-2.svg/9px-Lock-red-alt-2.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registration{color:#555}.mw-parser-output .cs1-subscription span,.mw-parser-output .cs1-registration span{border-bottom:1px dotted;cursor:help}.mw-parser-output .cs1-hidden-error{display:none;font-size:100%}.mw-parser-output .cs1-visible-error{font-size:100%}.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registration,.mw-parser-output .cs1-format{font-size:95%}.mw-parser-output .cs1-kern-left,.mw-parser-output .cs1-kern-wl-left{padding-left:0.2em}.mw-parser-output .cs1-kern-right,.mw-parser-output .cs1-kern-wl-right{padding-right:0.2em}
^ abcdefghijklm Dobbs, Matthew B.; Gurnett, Christina A. (18 February 2009). "Update on clubfoot: etiology and treatment". Clinical Orthopaedics and Related Research. 467 (5): 1146–1153. doi:10.1007/s11999-009-0734-9. ISSN 1528-1132. PMC 2664438. PMID 19224303.
^ Moses, Scott. "Clubfoot". www.fpnotebook.com. Archived from the original on 15 October 2017. Retrieved 15 October 2017.
^ ab "Talipes equinovarus". Genetic and Rare Diseases Information Center (GARD). 2017. Archived from the original on 15 October 2017. Retrieved 15 October 2017.
^ ab Miedzybrodzka, Z (January 2003). "Congenital talipes equinovarus (clubfoot): a disorder of the foot but not the hand". Journal of Anatomy. 202 (1): 37–42. doi:10.1046/j.1469-7580.2003.00147.x. PMC 1571059. PMID 12587918.
^ Weymouth, KS; Blanton, SH; Bamshad, MJ; Beck, AE; Alvarez, C; Richards, S; Gurnett, CA; Dobbs, MB; Barnes, D; Mitchell, LE; Hecht, JT (September 2011). "Variants in genes that encode muscle contractile proteins influence risk for isolated clubfoot". American Journal of Medical Genetics Part A. 155A (9): 2170–9. doi:10.1002/ajmg.a.34167. PMC 3158831. PMID 21834041.
^ Dobbs, MB; Gurnett, CA (January 2012). "Genetics of clubfoot". Journal of pediatric orthopedics. Part B. 21 (1): 7–9. doi:10.1097/BPB.0b013e328349927c. PMC 3229717. PMID 21817922.
^ ab AskMayoExpert & et al. Can clubfoot be diagnosed in utero? Rochester, Minn.: Mayo Foundation for Medical Education and Research; 2012. "Archived copy". Archived from the original on 2014-07-08. Retrieved 2014-08-13.CS1 maint: Archived copy as title (link)
^ Ganesan, B; Luximon, A; Al-Jumaily, A; Balasankar, SK; Naik, GR (2017). "Ponseti method in the management of clubfoot under 2 years of age: A systematic review". PLoS ONE. 12 (6): e0178299. doi:10.1371/journal.pone.0178299. PMC 5478104. PMID 28632733.
^ Gray, K; Pacey, V; Gibbons, P; Little, D; Burns, J (Aug 12, 2014). "Interventions for congenital talipes equinovarus (clubfoot)". The Cochrane Database of Systematic Reviews. 8: CD008602. doi:10.1002/14651858.CD008602.pub3. PMID 25117413.
^ Dobbs, Matthew B.; Nunley, R; Schoenecker, PL (May 2006). "Long-Term Follow-up of Patients with Clubfeet Treated with Extensive Soft-Tissue Release". The Journal of Bone and Joint Surgery. American Volume. 88 (5): 986–96. doi:10.2106/JBJS.E.00114. PMID 16651573.
External links
| Classification | D
|
|---|---|
| External resources |
|